The human body is a machine, and like any other machine- using our cars as a prime example, the more “kilometres put on the engine” the more wear and tear we are going to see on its individual parts. The expectation is, that over time, we will lose tread on our tyres, our break pads will wear down, and fluid levels will become low. When it comes to the human body, and the musculoskeletal system specifically, common areas susceptible to degenerative change (wear and tear) include the rotator cuff tendons of the shoulder, spinal discs, and knee joint cartilage- just to name a few.
Age-Related Change
We refer to this degenerative process as age-related change, a normal part of the ageing process that you could consider akin to developing wrinkles on the inside. Much like our cars, this is a natural process that occurs from putting “kilometres on the engine”, and much like our cars, our bodies can continue to function normally despite age-related changes, often without our knowledge that they even exist.
The Modern Medical Trap
Sometimes, often out of nowhere, and without any obvious inciting event, pain can develop in a region and may become persistent- leading an individual to seek medical opinion. There is a common misconception that persistent pain equals damage, and this thought may lead to referral for medical imaging such as X-ray or MRI scans to investigate further. Medical imaging techniques are used to detect anatomical abnormalities, which will inevitably be seen in most scans due to normal age-related changes. These abnormalities may then be incorrectly considered as the source of an individuals’ pain.
This is the beginning of the MODERN MEDICAL TRAP.
Treat the Man, Not the Scan
There are several common misconceptions that create the modern medical trap:
-
Persistent pain DOES NOT equal damage: Acute pain is short term pain, often directly related to an incident and may be associated with tissue damage, for example an ankle sprain while playing basketball. In this instance a scan may be appropriate to eliminate the possibility of a fracture and other associated injuries. Healing for acute pain usually takes less than 3 months, even in more severe injuries. Persistent pain however, lasts longer than acute pain, and may not even follow on from an acute incident. This type of pain is less to do with damage and sensitisation of tissues local to the injury site, and more to do with how pain is perceived by our brain and central nervous system. It is often referred to as the volume control of our pain system being stuck on LOUD.
For an excellent resource that explains the process behind persistent pain further, follow the link below:
Understanding Persistent Pain
- Findings on a scan DO NOT correlate with an individuals’ pain: The evidence of this is in the fact that age-related changes can also be asymptomatic, meaning that they can exist in an individual without there being any pain or loss of function, and therefore no awareness that these changes exist.
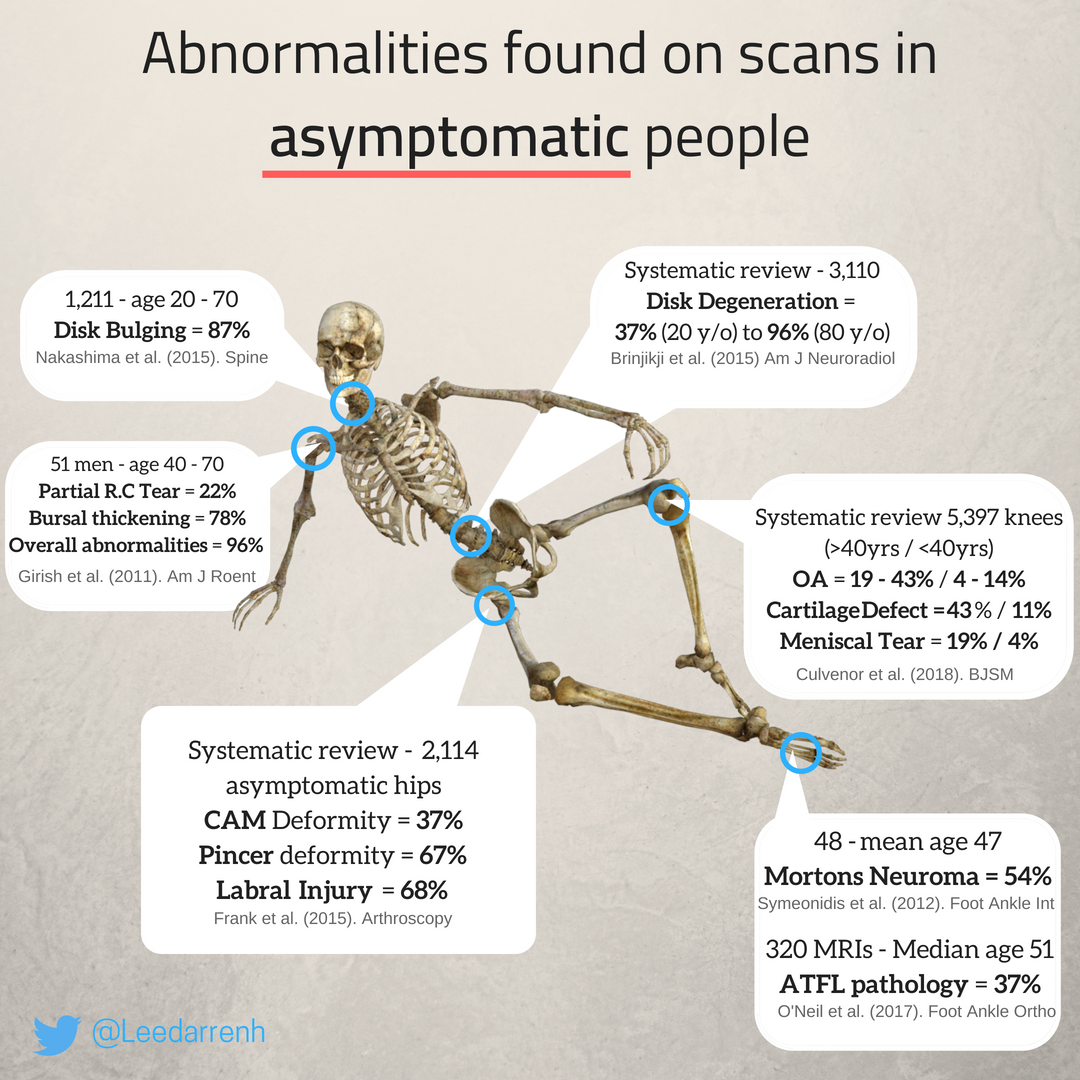
- Anatomical abnormalities found on a scan, are actually NORMAL: Using the lumbar spine as an example, findings seen on MRI scan may include disc degeneration, disc bulges, and facet joint degeneration. The table below depicts how common these actually are, and in patients who are asymptomatic!

The misconceptions surrounding persistent pain and the subsequent findings on medical imaging can create negative thought processes in an individual, leading to emotions such as fear and anxiety. This may in turn lead them to avoid physical activity, incorrectly believing it is harmful and will create further damage- when in fact being physically active is actually what they need. And when medical professionals suggest that normal age-related changes seen on medical imaging are responsible for their pain- this can lead to an individuals’ desire to receive corticosteroid injections or undergo surgical procedures to treat these “abnormalities” when they aren’t necessarily the source of the pain. All without having attempted more conservative forms of non-pharmaceutical, non-surgical management first.
So what conservative management options are available, and are they as effective as surgical and medical management? We answer these questions in Part 2...






